Table of Contents
HOW AND WHY DO SKIN TUMORS AND OTHER GROWTHS FORM?
Skin tumors (and cancers) are the most common malignant tumors. It must be remembered, the incidence of skin cancer and the changes that precede it (precancerous lesions) are increasingly taking on real epidemic proportions.
On the positive side, we already know a lot about them, thanks to a better understanding of the biology and pathology of tumors and the advancement of technology. Most important, fortunately, we can well control the newly created malignant changes in most cases with the help of relatively simple measures.
Generally, skin cancer occurs in the outer layer (epidermis), which makes it visible. Without a doubt, it mostly occurs on parts of the body exposed to the sun (scalp, face, lips, ears, neck, chest, arms, palms, but also the skin on the feet). The most common warning sign is a new change that is not healing.
Risk factors
- naturally brighter skin complexion
- family preference
- previously treated skin cancer in the same person
- excessive sun exposure (as part of an occupation but also a hobby)
- suffered burns in childhood or adolescence
- a type of skin that reddens slightly or gets burns, blemishes or becomes painful when exposed to the sun
- light eye color (blue, green), blonde or red hair
- certain types of moles and their excessive number
Most compelling evidence shows that well-known proven cause of skin cancer is ultraviolet (UV) radiation in the sun’s rays and commercial sunscreens (quartz lamps). To point out, it should be noted that both UVA and UVB contribute to the development of skin cancer. Consequently, the best way to prevent this is to protect yourself from the sun.
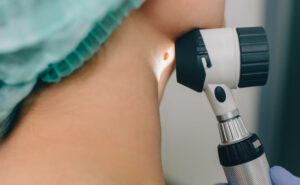
SUSPICIOUS LESION
The most common warning sign of possible skin cancer is a new change that does not heal.
Overall, cancer can manifest as a small, smooth, shiny, pale, or protruding lump. It can also occur as a reddish change. Occasionally there is a small spot of bleeding or scab. It can also appear as a formation at the level of the skin – reddish, rough, rough stain, dry consistency.
In the same way, there is also the so-called actinic keratosis, a change that looks like a rough, reddish, or brownish spot of various sizes that sometimes results in cancer. Obviously, characteristic of actinic keratosis is that it occurs in places exposed to the sun, but also elsewhere on the skin.
TYPES OF SKIN CANCER
Basically, there are three types of skin cancer:
Basal cell carcinoma (BCC), approximately 70-75% of cases. It usually spreads aggressively only locally, around the site of origin and grows very slowly
Squamous cell carcinoma (SCC), about 25% of cases, may be more aggressive and rarely spreads to local lymph nodes (metastases)
Malignant melanoma (MM), 1-5% of cases. This tumor can be very dangerous, with frequent development of regional and/or distant metastases
TREATMENT
If your doctor recommends, we perform surgical removal of the entire change (or slightly less often part of it). We call this procedure a biopsy. Subsequently, the tissue sample that we surgically remove is sent for pathohistological analysis (PHD). The pathologist checks what kind of change it is, ie. whether the removed change corresponds to the cancer.
To emphasize, it should be noted that the standard treatment of skin growths is complete surgical removal, i.e. excision. Undeniably, only a completely removed tumor guarantees a complete cure. In this sense, the surgeon’s task is to ensure safe (healthy) surgical borders. Of course, the aesthetics of the scar is certainly important, but not with the compromise of leaving remnant of the residual (rest) tumor.
The ideal type of removal may depend on the appearance and size of the cancer, the individual risk of scarring, age, and general health.
Surgical removal is the main and safest way. Surgeon removes the tumor with a secure healthy border that is typically a few millimeters. We close the resulting defect by primary suturing of the wound edges orwe can close it by “borrowing” tissue from the edge, ie. so called flap. Sometimes (in large lesions) a free transplant of healthy skin taken from another part of the body and we suture it into the resulting defect. There is also the possibility that the wound does not close at all, but that the heals with so-called secondary type of healing. For some regions on the face it is a very convenient way for the final appearance of the scar.
Excochleation and cauterization – under local anesthesia, we remove the cancer with a sharp instrument, and treat the surrounding tissue with a special instrument (electrocautery) to control bleeding and destroy any remnants of lesion around the borders of the wound. Most patients develop a flat, whitish scar upon completion of healing, no larger than the removed lesion.
So called cryosurgery (freezing with liquid nitrogen) for very small changes or actinic keratosis, often used by dermatologists.
Laser removal is sometimes used for tumors that affect very superficial parts of the skin. In similar cases, we can also perform a dermabrasion. OLn the negative side, it is not recommended for the removal of malignant changes due to the difficult pathohistological analysis of the borders.
Radiotherapy, a method used somewhat less frequently, in special cases and in places more difficult to access surgery
Topical chemotherapy with cream or lotion.
We emphasize that biopsy and pathohistological analysis (PHD) of a sample of altered skin is the only way to be sure with certainty whether it is cancer.
POSTOPERATIVE CONTROLS
In brief, postoperative controls are mandatory for all skin cancers. It must be remebered, according to some data, there is as much as a 50% chance that other skin cancer will occur after the first one is removed. With this in mind, the recommended time for regular check-ups is approximately 3-5 years after removal of the first tumor.
SKIN CANCER PREVENTION
To conclude, there are 5 most important ways to protect against skin cancer:
- Avoiding excessive sun exposure, staying in the shade, especially in the noon hours (10-16 h) when UV rays are the strongest and most harmful
- Covering the skin with clothes and shoes
- Wear headgear (hat, scarf) or covering head, ears and neck
- Umbrellas that provide approximately 100% UVA and UVB protection
- Apply sunscreen or oil (SPF) 15 or more