Tonsillectomy and adenoidectomy
Table of Contents
DIAGNOSTIC AND THERAPEUTIC APPROACH
Tonsillectomy and adenoidectomy is a common topic in ENT clinics, chiefly pediatric. Most often, the conversation begins with data on inflammatory diseases. Inflammation of the throat and sore throat in most cases is of viral etiology. Much less often it is bacterial (beta-hemolytic streptococcus group A as the most common cause).
Consequently, the key diagnostic task is to distinguish bacterial infection (in which the use of antibiotics is justified) from many other sore throats. In other non-bacterial cases the use of antibiotics will not have a significant impact on the course of the disease. Contrarily, it may contribute to the development of bacterial resistance to antibiotics. Hence the Guidelines of the Interdisciplinary Section for the Control of Antibiotic Resistance (ISKRA) of the Ministry of Health and Social Welfare of of Croatia help us in this. Shortly, the Task Group created guidelines in accordance with the principles of the AGREE (Appraisal of Guidelines for Research and Evaluation) methodology. This implies that they are the result of a consensus of professional societies and institutions.
In the diagnosis of streptococcal sore throat, it is recommended to evaluate the clinical picture according to the so-called Centor’s criteria. Basically we do not recommend antibiotic therapy and bacteriological testing for patients with 0–1 points. For patients with a score of 2 to 4, we recommend to do bacteriological testing (rapid test or culture). In case of a positive bacteriological test, we prescribe antibiotic therapy.
Most important, the first drug of choice in the treatment of streptococcal tonsillopharyngitis is penicillin. It is administered orally for 10 days (penicillin V). In case of poor patient compliance, we give it once parenterally (benzathine penicillin G). We use other antibiotics exceptionally in cases of hypersensitivity to penicillin or in recurrent infections. These are mostly macrolides, clindamycin, cephalosporins, co-amoxiclav).
Tonsillectomy and adenoidectomy represent a surgical modality of treatment, in addition to the already mentioned conservative measures or as a stand-alone procedure.
TONSILAR PROBLEM
Tonsillar problem is a common name for a number of issues related to the correct and timely setting of indications for surgical treatment of tonsils. To sum, these questions are aimed at assessing the state of the tonsillar tissue. We take data on tonsil disease and possible complications of these diseases into account here. We also consider local findings that we obtain by clinical examination (hypertrophy and appearance of tonsillar tissue).
The guidelines help us decide more easily about the two main indications for surgical treatment. These are:
- hypertrophy (enlargement) of the tonsils and
- frequent inflammation.

TONSILLECTOMY AND ADENOIDECTOMY GUIDELINES
Tonsillectomy is an accepted surgical method that reduces the number of sore throats in children and adults, but only if we follow the indications for the procedure.
Overall it is a surgical method for which the hospitalization is obligatory. We perform the procedure in children under general anesthesia, and in adults also under local anesthesia, although currently very rarely. The most common postoperative complication is bleeding (1-3%). Postoperative recovery lasts 14 days and during that time the patient is absent from school or work.
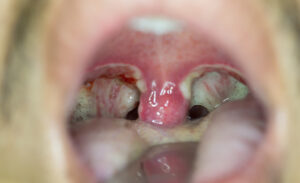
Absolute indications (reasons for surgery)
- sore throat caused by tonsillitis with the following conditions met: 5 or more episodes of sore throat per year (positive swab on BHS-A, purulent exudate on the tonsils, body temperature ≥ 38 ° C, lymphadenitis of the neck with at least one node ≥ 2 cm)
- episodes of sore throat affect the general condition of the patient and his normal functioning in daily life
- complications of tonsillitis (peritonsillar abscess, sepsis)
- permanent airway obstruction
- obstructive sleep apnea syndrome (OSAS)
- suspected malignant tonsils
Relative indications
- occlusion disorders (bite)
- chronic tonsillitis (chronic sore throat and bad breath)
We recommend a six-month follow-up period before deciding on tonsillectomy. Once we set the indication, it is necessary to perform the procedure as soon as possible in order to achieve as much success as possible.
Tonsillotomy (partial tonsillectomy, intracapsular tonsillectomy, subtotal tonsillectomy) is an alternative method to tonsillectomy. It causes less postoperative pain and a lower risk of postoperative bleeding, enables faster recovery and return to normal physical activity and eating habits.
As the reduction of postoperative morbidity after surgery of the palatine tonsils is the main goal, it is obvious that the popularity of intracapsular tonsillectomy is growing significantly. It is especially common in some countries such as UK where it is used in numerous medical centers as the exclusive method of surgery.
POTENTIAL COMPLICATIONS AND PROBLEMS
Potential disadvantages of surgical treatment are residual tissue in the tonsillar fossa (incomplete removal of the tonsils) which poses a risk for reoperation.
Re-growth of tonsillar tissue was recorded in 0 – 4.7% of operated patients, regardless of the indication and technique of operation (laser, radiofrequency, microdebrider). The need for reoperation occurs in 2.5% of cases regardless of the indication.
Risk factors for regrowth of tonsils after tonsillotomy are:
- a large amount of sugar in the diet
- frequent respiratory infections of the upper respiratory tract
- age of primary surgery before the third year of life
The same conclusions apply to the adult population whose indication is hypertrophic tonsillitis with or without sleep-disordered breathing.
Tonsillotomy or tonsillectomy is recommended for all absolute and relative indications for surgery, and additional consultation with parents or adult patients is certainly required in which the advantages and disadvantages of each of the methods are highlighted.
The literature confirms that the results of surgical treatment of tonsillectomy and tonsillotomy are completely equal in terms of increasing quality of life, reducing sleep-disordered breathing, and reducing the number of throat infections.